Study: Electronic prescribing improves quality of medical treatment

E-prescribing reduces the co-prescribing of harmful drug-combinations. This is according to a new study using comprehensive administrative data and the staggered introduction of a nationwide electronic prescribing system in Finland.

Illustration
In fragmented healthcare systems, a patient’s care delivery is spread across multiple healthcare organizations and physicians, and each physician has different knowledge of the patient’s medical history. The central goal of health information systems such as e-prescribing is to improve coordination between the different parties involved in a patient’s care.
Fragmentation can result in coordination failures, such as the co-prescribing of harmful drug combination. The combination of blood thinners and anti-inflammatory drugs (NSAIDS), known to increase the risk of major bleeding complications, is one of the most common and harmful combinations of prescription drugs.
Nationwide roll-out of e-prescribing demonstrates the benefits information integration
Researchers from the VATT Institute for Economic Research, University of Jyväskylä, University of Turku, and the University of Pennsylvania study how the introduction of a nationwide e-prescribing system in Finland impacted the co-prescribing of Warfarin, a common blood thinner, and anti-inflammatory drugs, such as ibuprofen and aspirin.
The researchers use comprehensive administrative data on over 1.7 million prescriptions to over 250 000 Warfarin users between the years 2007 and 2014. They find that the introduction of e-prescribing reduced the co-prescribing of harmful drug combinations in previously low-performing (rural) regions.
- Electronic prescribing can improve the quality of medical treatment. In comparison to providers’ pre-existing incompatible health information systems, the e-prescribing systems allowed physicians involved in a patient’s care to obtain more comprehensive information on prescriptions. Our results demonstrate the potential of such integrated information systems in mitigating coordination failures and improving the quality of care, says Senior Researcher Tanja Saxell from VATT.
The analysis is based on a staggered roll-out of the e-prescribing system across all municipalities in Finland between 2010-2014.
- The adoption time of the e-prescribing system in different regions was determined by technical reasons rather than underlying trends in prescribing or health outcomes. This enables us to reliably study the effects of e-prescribing on the quality of prescribing, says Professor Petri Böckerman from the University of Jyväskylä.
Largest improvements in rural regions
Prior to e-prescribing, co-prescribing Warfarin and NSAIDS was fairly common in Fin-land: the regional share of interacting prescriptions was 6 percent on average, with substantial variation across municipalities (between 2 and 19 percent). Nearly 80 percent of the worst performing municipalities, as measured by the fourth quartile of the regional interaction share, were rural.
According to the study, e-prescribing reduces the harmful co-prescribing of Warfarin and NSAIDS by nearly 35 percent in rural municipalities (Figure 1). The main driver behind this reduction is the improvement in the quality of prescribing by unspecialized physicians (general practitioners) in rural regions. In more urban regions, no statistically significant effect is observed.
- A plausible explanation for the results is that the lack of specialised physicians in rural regions not only limits access to specialist medical services, but also the ability of general practitioners to consult and learn from specialists, argues Doctoral Candidate Mikko Nurminen from the University of Turku.
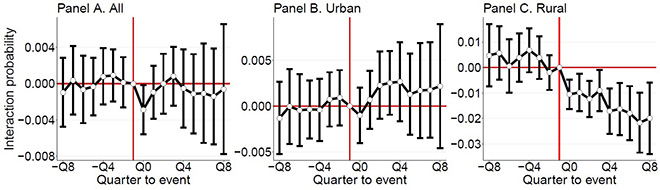
Figure 1. In rural municipalities, the co-prescribing of Warfarin and NSAIDs was reduced by nearly 35 percent compared to the mean following the introduction of e-prescribing.
Improving coordination between physicians
Prior to the reform, over a half of a patient’s prescriptions were obtained from a different physician than previously.
- Improving information flows between physicians involved in a patient’s care was the main driver behind the overall improvement in the quality prescribing. This effect is notable particularly in rural regions, says Postdoctoral Researcher Liisa T. Laine from the University of Pennsylvania.
The study demonstrates the potential of health information technology in improving coordination and mitigating the harms of fragmentation in healthcare. The usability of these systems is also important.
- The lack of easy and user-friendly access to a patient’s complete and up-to-date medical records can reduce the potential benefits of information integration. The system could be further improved by introducing automatic tracking of all currently used medications and detection of prescriptions errors, the authors note.
Research:
Petri Böckerman, Liisa T. Laine, Mikko Nurminen ja Tanja Saxell (2020) Information Integration, Coordination Failures, and Quality of Prescribing. VATT Working Papers 135.
More information:
Senior researcher Tanja Saxell, VATT Institute for Economic Research, Tel. +358 295519 460;
Postdoctoral researcher Liisa T. Laine, University of Pennsylvania, Tel. +1 617 901 8474;
Doctoral candidate Mikko Nurminen, University of Turku;
Professor Petri Böckerman, University of Jyväskylä, Tel. +358 400 913189;
Tanja Saxell
Healthcare services Local public finance and provision of public services Press release Uutiset ja tiedotteet adverse drug reactions efficiency of public services electronic prescription health and social services health economics health economics healthcare pharmaceutical markets public services

